As 17th November is World Prematurity Day, I thought it would be great to do a post based on preterm nutrition.
In the UK, it is estimated that 600,000 babies will be born prematurely every year, approximately 1 in every 13 births. This is defined as a baby who is born before 37 weeks gestation. In the final trimester of pregnancy, this is a period of growth and laying down fat stores.
Feeding your premature baby
Breastmilk is recommended for all infants as this is bespoke nutrition for each individual baby as well as containing many non nutritive benefits like probiotics, antibodies and hormones.
The first milk is colostrum. This is a nutrient rich liquid containing all the nutrients that your baby needs in the first few days of life. Breastmilk supply generally increases around day 3-4 when colostrum changes to mature milk.
It is not possible for all mothers to breastfeed their babies. If this is the case for you, the neonatal team who are caring for your baby, will discuss and decide on the appropriate feeding choice for your baby.
Feeding development + routes of feeding in preterm nutrition
The sucking reflex is fully developed around 36 weeks gestation. For babies born earlier than this, they may require alternative feeding than breast or bottle. Some babies may be offered cup feeding if appropriate, while babies born at less than 36 weeks gestation may require tube feeding for their feeds to enable them to grow and develop.
For some babies, feeding enterally (via a tube that goes down into the stomach) may not be possible and intravenous nutrition may be advised by the team.
Growth measurements
Babies who are born prematurely will have their growth plotted on different growth charts or will have it plotted based on their corrected age.This means that their growth will always be measured taking into account the weeks + days that they were born early (based on 40 weeks gestation).
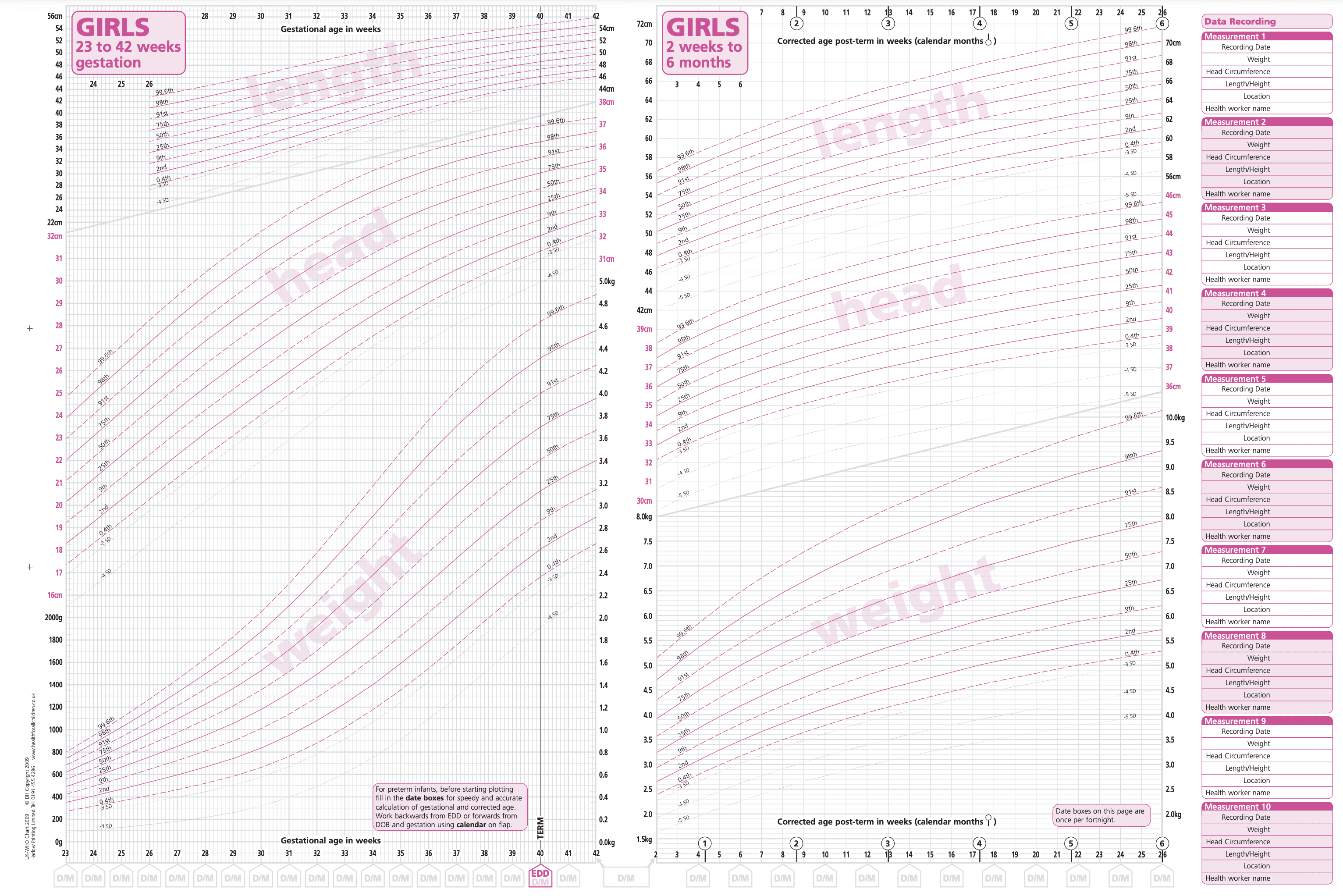
Some babies will have increased nutritional requirements which may require monitoring and adjustments to their feeding plan. Please always liaise with the medical and dietetic team should you have any questions.
Introduction of complementary nutrition (weaning)
It is recommended that all babies commence complementary feeding when they show signs of readiness. This includes being able to hold their head steady, sit with support and show interest in food or other eating.
Great foods to include when starting weaning include
- Vegetables including broccoli, avocado and carrots
- Iron rich foods including red meat, beans and pulses
- Fruits including apples, pears and banana
- Carbohydrate foods like oats, potatoes and rice
- Dairy foods including plant based options that are fortified including yoghurts and cheese
We will do a detailed post on weaning soon but if you have any questions, please feel free contact The Gut Health Clinic and request an appointment with Chloe Elliott, a paediatric speacialist dietitian within the team.
There is also great information available from Bliss, a charity with information to help those children who are born sick or prematurely.