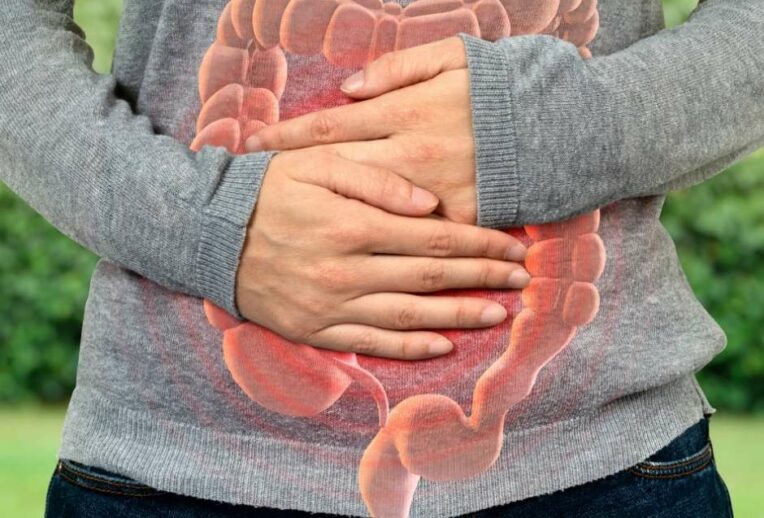
Around 1 in 1000 people in the UK have microscopic colitis. However, this is likely to be an underestimate as the diagnosis can be difficult. It often results in a misdiagnosis of IBS-D or diverticulitis.
What is microscopic colitis?
Microscopic colitis is a form of inflammatory bowel disease (IBD). It is slightly less well known than the more common forms of IBD: ulcerative colitis and crohn’s disease. It is characterised by superficial inflammation of the colonic (large intestinal) lining. Unlike crohn’s disease or colitis, it is the inner lining of the colon that is affected. This cannot be seen during a colonoscopy (a camera which allows us to see into the colon and view its lining). Unlike other forms of IBD, microscopic colitis does not put you at an increased risk of developing colon cancer.
There are 3 main types of microscopic colitis, however, symptoms and treatment are the same:
- Lymphocytic (the inner lining has more white blood cells than usual, these are produced as an inflammatory response). Coeliac disease can be associated with this type of microscopic colitis.
- Collagenous (a thickened protein layer of collagen develops), there may also be an increased number of lymphocytes
- Incomplete is a slightly newer term and refers to patients who have the classic symptoms of microscopic colitis as well as abnormal tissue under a microscopy, but who do not fit into one of the above two classic criteriums
What are the symptoms:
The main symptoms in microscopic colitis include:
- Frequent watery stools/diarrhoea which can be multiple times/day and in the night
- Fatigue
- Weight loss
- Joint pain
- Bloating and wind
- Abdominal cramping (lower)
Many of the above symptoms are common amongst gastrointestinal conditions and so you can see why this condition can be easily misdiagnosed!
The main role of your colon is to reabsorb water and electrolytes, such as potassium and sodium. If the lining of your colon is inflamed and not working efficiently, much of the water that should be reabsorbed is instead lost alongside these electrolytes.
Unlike ulcerative colitis, blood in the stool is not usually a symptom of microscopic colitis.
Causes and risk factors:
The causes of microscopic colitis are unknown. It is thought that some medications could contribute towards its development, predominantly PPIs (especially lansoprazole), SSRIs (e.g. citalopram, sertraline) and NSAIDs (e.g. ibuprofen, naproxen). These can all irritate the colonic lining, resulting in inflammation. That said, these medications are extremely important for some people and should not be stopped or reduced without the guidance of a doctor.
Microscopic colitis can also be caused by inflammation due to bile acid diarrhoea (BAD). Bile acids are released to help you digest fats in the diet and should be reabsorbed before they reach your colon, but if they are not, they can enter the colon and cause irritation. Sometimes a scan called a SeHCAT scan is used to diagnose this.
There are also uncontrollable risk factors which may increase the likelihood of developing microscopic colitis. These include genetics, age (50-70 is the main age of development) and female gender. If you have an autoimmune disease such as coeliac disease or multiple sclerosis, you are also at an increased risk of developing microscopic colitis.
Diagnosis:
If you are having gastrointestinal symptoms, it is important to first visit your GP who can complete a coeliac screen as well as test for markers of inflammation within the blood. A stool test called faecal calprotectin is often indicated with frequent loose/watery stools. This stool test is a marker of inflammation which is often raised in the presence of crohn’s disease or ulcerative colitis but may only be slightly raised or not raised at all in the case of microscopic colitis. To further complicate matters, as the inflammation is so small (microscopic), it cannot be seen with a colonoscopy or endoscopy. Instead, a small segment of tissue (biopsy) must be taken and looked at under a microscope to diagnose this condition.
Treatment:
Medication is often the first line treatment, based on what is thought to be an underlying cause. You may have a scan to assess for BAD. In that case medications called sequestrants may be prescribed to bind the bile acids which are not being reabsorbed, preventing them from irritating the colon wall. An alternative medication which has good intervention trials behind it is called budesonide, which is a type of steroid. This has been shown to be effective against placebo and mesalazine, which is an alternative medication used to treat other forms of IBD. The relapse rate after discontinuing budesonide can be high. 62% of patients relapse after treatment, usually within 3 months. Some people will be advised to taper down and continue to take budesonide as a low dose maintenance therapy.
Other treatments may include immunosuppressants or biologics, which are also used in other forms of IBD.
Diet and microscopic colitis:
Diet can be used to help control symptoms whilst awaiting or beginning medical treatment. Sometimes a temporary low fibre or low-fat diet can be helpful. This is very individual and should be discussed with your dietitian. Those with microscopic colitis are also more than 50 times more likely than the general population to have or develop coeliac disease. Therefore, this should be tested for before any exclusion of gluten is made.
After treatment, it is key to maintain a healthy diet including a variety of plant-based products to help to optimise and strengthen your gut health.
If you are worried about gastrointestinal symptoms, your first port of call is always your GP who can then refer you to a gastroenterologist if necessary.